Introduction
Parkinson’s disease (PD) is a degenerative condition of the central nervous system that most commonly affects the motor system. The assignment’s goal is to raise awareness of PD and sickness prevention among UK males aged 50 to 60. The assignment begins with a justification that supports the professional reason for picking the topic and population. It then moves on to a background examination of PD health difficulties, defining the challenge and identifying various types and causes utilizing literature evidence. It then examines epidemiology, focusing on the causes, trends, and consequences in the defined population. It then examines the nurse’s assessment of the health promotion components of PD. Later, the nursing goals, health promotion targets to reach, and intervention approaches are evaluated. The interventions address the health promotion strategies used for the PD promotional campaign. A critical review of the intervention, assessment, and goals is then presented, along with recommendations for improvement. The assignment closes by summarizing essential elements and indicating how the information will benefit professional growth.
Rationale
Parkinson’s disease becomes more prevalent as people get older. According to the PD Society of the UK, men have a greater prevalence of Parkinson’s than women. Men aged 50 to 89 had a 1.5 times greater frequency than women in the same age range. PD is a degenerative condition of the central nervous system that most commonly affects the motor system. Non-motor indications and symptoms are typical as the illness progresses. The signs and symptoms of this condition develop progressively over time. In the early stages, symptoms include stiffness, tremors, sluggish movements, and walking difficulty. Problems with behaviour and cognition may also arise. Patients with severe Parkinson’s disease frequently develop dementia. Anxiety and despair are also quite frequent. Imagine being unable to move, sleep, or smile. Feeling nervous or sad and unable to think or recall. Your body does not feel like your own. Parkinson’s might make you feel like this. According to the PD Society of the UK, someone in the UK is diagnosed with PD every hour – a brain ailment that upends people’s lives and leaves them worried about the future.
The fact that the UK is one of six nations with the most significant prevalence of PD in Europe gives ample basis for picking the topic. Furthermore, the majority of patients with PD in Wales are above the age of 50. The health promotion approach will empower the targeted community with knowledge spanning from early screening to treating PD if positively diagnosed, among other healthcare initiatives. Furthermore, health promotion would enable me to carry out my duty as a nurse practitioner, which is to reposition medical care and enhance community health action. According to Torre et al. (2016), documenting incidents and trends might help make an informed decision. The PD topic would include extensive research and information on the subject. I have seen family members and intimate friends struggle with PD. I am interested in PD situations because I intend to work in the UK’s PD research centre. Therefore, skills, information, and study on the illness would be vital in my current and future healthcare goals.
Background
PD is a neurodegenerative condition marked by the gradual loss of dopaminergic neurons. It is a chronic multisystem condition that manifests in a wide range of motor and non-motor symptoms. These non-motor symptoms occur frequently and become more common as the disease progresses. It is a clinical condition distinguished by the following features: gradual slowing of voluntary movement (bradykinesia), muscle rigidity, stooped posture, and a unique gait with short accelerating steps. Reduced facial expressiveness and resting tremor. Dopamine, a neurotransmitter that is ordinarily synthesized and stored in the basal ganglia of the midbrain, is depleted due to degeneration of the substantia nigra. Dopamine facilitates the control of motor function and facilitates intentional, fluid motions. Dopamine deficiency impairs the extrapyramidal tracts, which results in a loss of motor coordination. Fall-related injuries and loss of independence are examples of complications that significantly lower quality of life.
Epidemiology
The study of health and illness conditions in a population’s trends, causes, and consequences is known as epidemiology. It displays the distribution of health and the factors that influence health-related incidents. Epidemiology is crucial because it gives nurses information that helps them understand aetiology, guide evidence-based practice in healthcare interventions, and shape policy decisions.
PD is the world’s fastest-growing neurological ailment, with one out of every 37 individuals in the UK expecting to be diagnosed with it at some point in their lives (Parkinson’s UK, 2020). In the UK, over150,000 people are already living with Parkinson’s disease, with estimates128,000, 12,900, 8,300, and 4,200 for 2023 in England, Scotland, Wales, and Northern Ireland, respectively (Parkinson’s UK, 2020). With population growth and ageing, this figure is expected to rise to over 170,000 persons by 2030. The number of people with PD under the age of 50 is estimated to be 1,800, with 1.2% of those diagnosed being under 50 (Parkinson’s UK, 2020). Men are more prone than women to develop the illness, which a mix of biological and lifestyle factors could explain. Men aged 50 to 89 had a 1.4 times higher risk of developing PD than women. There is a growing need to learn more about the risk factors and the natural history of PD as the condition becomes older and more common in industrialized economies. The extent to which the disease has spread within a particular population and the information available regarding the risks of contracting the disease can both be inferred from the epidemiology (prevalence and incidences) of PD (Noyce et al., 2016). In the UK, the prevalence of PD is generally estimated to be 0.3% of the total population and approximately 1% of those 60 years of age and older. Men are more likely to be affected than women. The prevalence estimates differ depending on the region; among populations aged 89-95, Europe reported a 3.5% prevalence estimate.
Assessment
The method that nurses and other caregivers use to provide high-quality, patient-centred care successfully is known as nursing assessment in care planning. There are five steps involved in this process: assessment, diagnosis, planning, execution, and evaluation. There are various ways that PD is diagnosed. No test can definitively determine that you have PD, according to the NHS. A thorough physical examination, your medical history, and your symptoms will all be used by the doctor to make a diagnosis. (NHS, 2022). In order to aid in the diagnosis, the general practitioner will speak with the patient about their issues and might urge them to carry out a few easy physical or mental exercises, such as moving or strolling. Because symptoms are usually modest in the early stages, it may be difficult for the GP to determine whether you have the ailment for sure. In the event that the general practitioner detects Parkinson’s disease, a specialist will be consulted. This will typically be a geriatrician, a neurologist, or an expert in issues affecting the elderly, depending on the ailment affecting the brain and neurological system. The physician will have the patient complete a series of physical tests in order to determine whether mobility issues are present. In certain situations, specific brain scans, including a single photon emission computed tomography (SPECT) scan, might also be performed in an effort to rule out alternative reasons for your symptoms (NHS, 2022).
Health Promotion Model
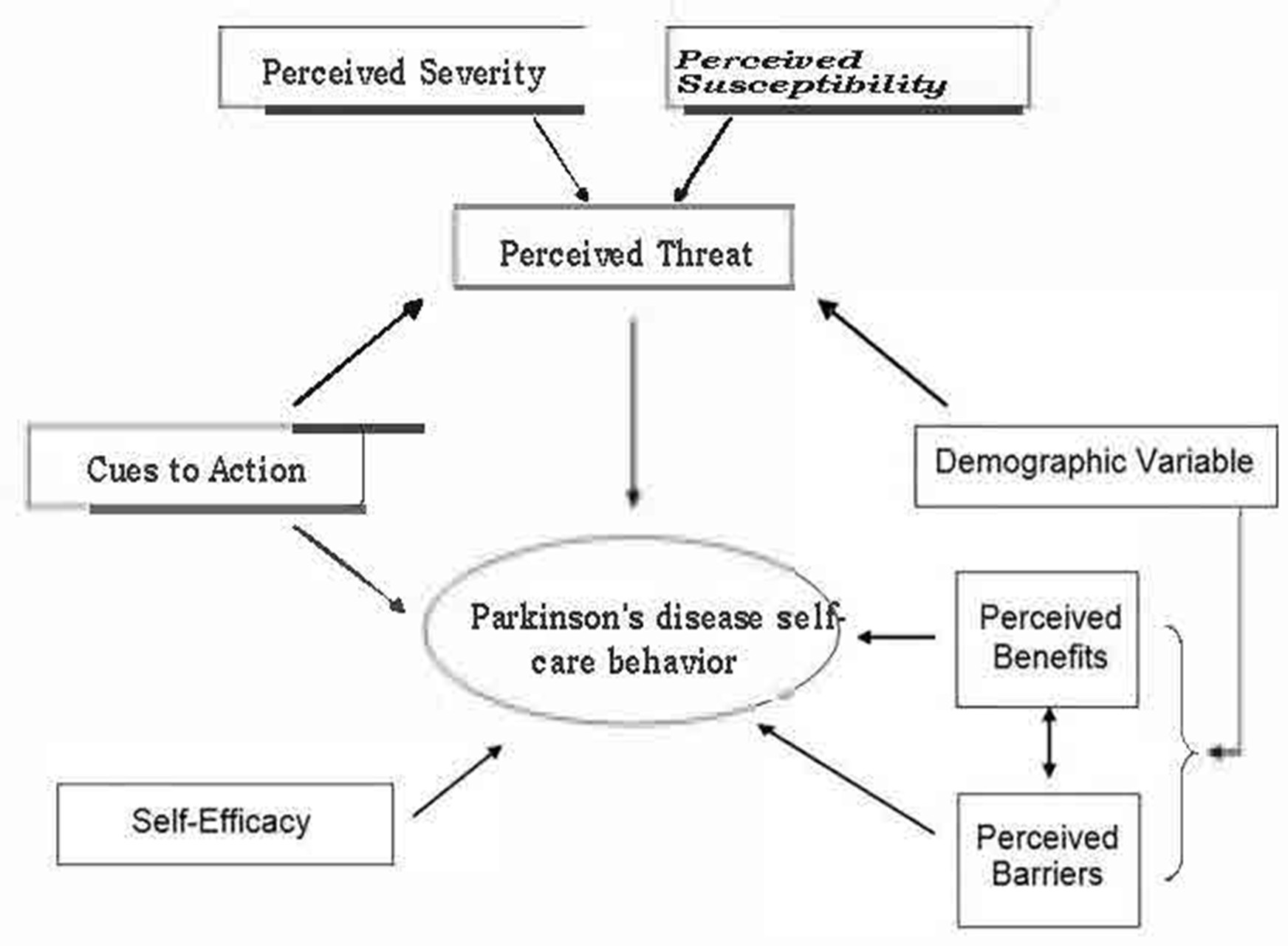
For caregivers to guarantee and assist in the avoidance of illness and the promotion of health in the healthcare industry, a variety of health promotion models are employed. In order to define and establish goals and interventions, programs that help understand and explain health behaviour are planned using the health promotion models, which are helpful in the healthcare industry. When selecting a theory or model to direct health promotion or disease prevention initiatives, it is critical to take into account a number of factors, such as the particular health issue being addressed, the population or populations served, and the program’s implementation environment (Green et al., 2020I will use the health belief model in health promotion to help tackle the problem of PD in the UK. A psychological model called the Health Belief Model (HBM) aids caregivers in comprehending the decisions and behaviours related to their patient’s health. As a caregiver, I have seen from the model that health-related behaviours can be influenced by an individual’s belief in their risk of sickness, their understanding of the advantages of getting medical help to lessen that risk, and the obstacles to getting medical aid. When used in relation to PD, the Health Belief Model (HBM) will enable me to comprehend how people view their likelihood of contracting the illness, their opinions on the efficacy of the interventions I will provide, and the obstacles they encounter in managing the condition. It can assist me in creating treatments that are specifically designed to address these elements, ultimately leading to improved outcomes and management for persons who have Parkinson’s disease.
Goals
The process of creating targets that assist nurses and other caregivers in determining whether their needs have been fulfilled is known as goal setting in nursing care planning. The campaign’s objectives for health promotion are to:
- To provide a free CBT Helpline and connect with at least 25% of Parkinson’s patients in the UK who also experience depression and anxiety.
- To support remote trials as a type of social care in order to assist more people with PD in carrying out everyday activities and preserving their independence and general well-being
- In the next six months, increase by more than 15% the proportion of males engaging in combined positive lifestyle changes—exercising and eating healthily—as a preventive measure against PD.
In order to promote health and avoid PD, each of the objectives above is crucial. According to Todd et al. (2016), the first goal would lead to fewer incidents and a decrease in the resources used for social and health care. When it comes to early detection of and referral to social care, health practitioners can play a crucial role. The second objective is to lower the chance of acquiring PD and potentially change the condition. Motor parkinsonism can be stabilized by exercise, albeit this may also be a symptomatic effect. Exercise is also a workable strategy because of its low risk of adverse effects. Because the various physiological processes may have an additive or even synergistic effect, combining interventions like exercise and a balanced diet could increase their effectiveness (Janssen Daalen et al., 2022). In addition to improving the scalability of lifestyle interventions, remote administration may help with diversity by allowing more geographically isolated and other difficult-to-reach people to be included.
Interventions
The act of implementing measures and taking action to solve a healthcare condition utilizing alternative solutions is known as intervention in the nursing process. The intervention to reduce PD in improving health and preventing illnesses would encourage the implementation of various healthcare approaches to effectively achieve established goals, as indicated in the aims previously mentioned.
The three interventions in the PD case explore what constitutes high-quality social care for Parkinson’s disease patients and their caregivers. In order to avoid PD, more men should adopt a combined positive lifestyle that includes eating well and exercising. Additionally, faithfulness, treatment implementation, and the experiences of an occupational therapy intervention in PD should be assessed. The three strategies for encouraging healthy individuals and groups are the medical or preventive strategy, the behavioural change strategy, and the social change strategy. The empowerment approach likewise covers the case intervention for promoting home-based interventions. Men would learn the value of early detection from it. The targeted women would have more authority over their lives as a result.
The nursing interventions for each aim would involve implementing distinct strategies to facilitate and guarantee that the three objectives mentioned are accomplished within the allotted time frames. The initial objective would be to implement secondary preventive nursing intervention by offering a free CBT Helpline to Parkinson’s patients in the UK who also experience anxiety and depression. CBT, or cognitive behavioural therapy, is one treatment option for Parkinson’s depression. According to research conducted in Italy, people with PD who have mental health issues common to all psychological diseases can benefit from cognitive behavioural therapy (CBT), which is known to be an effective method for lowering apathy and depression in the patient (Berardelli et al., 2018). Providing patients with the chance to engage with other patients and exchange knowledge and experiences is the fundamental idea behind CBT. The patient’s neurological and psychological problems can also be treated with CBT. Twenty Parkinson’s patients participated in a 12-week trial, and the results indicated that the intervention was effective because the participants’ levels of anxiety and depression had decreased. CBT can be conducted in person or over the phone. People with anxiety who may find it particularly difficult to discuss personal topics in person can benefit significantly from telephone therapy. The therapist will typically start a session by probing you with questions to learn more about your most uncomfortable situations and environments, your coping mechanisms, and how anxiety impacts your day-to-day functioning. To determine whether you have mild, moderate, or severe anxiety, they will usually utilize a scoring or charting system. They will then follow this information week by week. Therapists will collaborate with you to determine the causes of your unfavourable or anxious emotions and how they influence your behaviour. Exercises and assignments to assist you in altering your perspective and reassessing your circumstances in order to get a different result will be provided to you in between sessions.
The second would be to promote remote trials as a kind of social care in order to assist more people with PD in carrying out activities of daily living and preserving their independence and general well-being. Home-based trials are the best option for preventing PD since they have the potential to have a higher participant base and fewer exclusions. Lifestyle interventions can be administered remotely to improve scalability and tackle diversity concerns. Group therapy can be administered remotely, and home-based therapy can stabilize the course of motor symptoms. Trials of home-based lifestyles can be successful in low-socioeconomic areas without requiring expensive equipment. Digital technology, such as body-worn sensors or connected devices, can be used to measure the results of exercise. Exercise levels can be automatically measured remotely, allowing enabling data analysis and immediate feedback. Patient-reported outcomes can be gathered using digital diaries, facilitating direct contact and automatic compliance calculations.
The third objective would be to increase by over 15% during the next six months the proportion of males engaging in combined positive lifestyle changes—exercising and eating healthily—as a preventive measure against PD. Exercise has been associated with a lower risk of developing PD in the future. Non-pharmacological therapies for PD management also take nutrition and exercise into account, as well as how these factors affect the disease’s course and general quality of life. Regular physical activity has been linked to several benefits in PD (Sharpe et al., 2020). These benefits include weight training, flexibility exercises, and aerobic workouts. Exercise may have a neuroprotective effect on the underlying pathophysiology of disease in addition to improving motor function. Also, according to Sharpe et al. (2020), the diets support brain health in those with Parkinson’s disease. While there is not a set diet for PD, research has indicated that specific dietary approaches, such as the Mediterranean diet high in omega-3 fatty acids and antioxidants, can affect the severity and course of the condition (Franco et al., 2023). The gut-brain axis in PD and its implications for therapeutic approaches are being studied in ongoing research, taking into account the possible link between gut health and food. The inclusion of these lifestyle adjustments in the treatment plan highlights the complexity of managing PD and the value of combining pharmaceutical and non-pharmacological methods to enhance patient results.
Evaluation
In order to evaluate the effectiveness of the interventions used and determine whether the objectives have been met, the evaluation of diabetic prevention measures is essential. Assessing patient satisfaction levels is one of the metrics used to determine the effectiveness of therapies. Did the clients feel satisfied with the care they received?
Verifying patient readmission and admission can be helpful in assessing the effectiveness of interventions aimed at lowering comorbidity and mortality related to problems with Parkinson’s disease. Were telemedicine-based therapies aimed at closely monitoring patients successful? Did the medical system contact patients who lived in a rural area? Were the patients provided with information and awareness? Reducing patient readmissions to the hospital as a result of PD problems is necessary to comprehend this. Determining the effectiveness of the interventions can be aided by looking up national data on mortality related to complications from diabetes. Another critical measure of the effectiveness of the therapies is the decrease in emergency services for PD complications. Overall, fewer people should die from PD-related complications as a result of the therapies.
Caregivers should ascertain whether patients exhibit better depression, anxiety, sleep disturbances, and specific other non-motor symptoms in patients with PD in order to assess the effectiveness of cognitive behavioural therapy (CBT). Caregivers should show that CBT significantly reduced non-motor symptoms associated with Parkinson’s disease. Does CBT help PD patients with their anxiety and depression scores? RCT trials with long-term interventions are required to investigate the effects of CBT in more detail. Additionally, we may evaluate if the effect sizes of offline and online interventions are almost identical. However, due to patients’ physical disabilities and other issues, face-to-face CBT has limitations in terms of clinician-patient engagement. One way to evaluate the effectiveness of social care provision is to look at what individuals with PD and their carers consider to be high-quality social care and how it affects their health and well-being.
Sadly, it may take several months for the NHS to send patients for CBT. This means that if prompt assistance is not provided, a person with PD may experience a simultaneous and rapid decline in both their physical and emotional wellness. Parkinson’s patients who also suffer from anxiety or depression may also experience the following symptoms: increased tremors, decreased mobility as a result of stiffness and tension, sleep disturbances like insomnia that can lead to further hallucinations and cognitive decline, and an inability to exercise as a result of extreme exhaustion and lack of motivation. Not all NHS therapists have expertise in treating patients with neurological diseases like PD with psychotherapy. Psychotherapy and neurobiology are combined in neurological psychotherapy. It is grounded in science and focuses on the anatomy, physiology, and connections between neurons in the brain.
The following suggestions are offered to enhance the healthcare promotion initiatives related to PD interventions.
- Collaborating across disciplines with many stakeholders, including the private and voluntary sectors, can foster the prevention of diabetes and promote overall health.
- Indicate the influence that additional healthcare promotion strategies would have in order to compare and choose the best ones.
- Use research to support the most effective intervention chosen to work in the specified age group and gender, such as the communication plan to accomplish the goal.
Conclusion
The goal of the presentation was to introduce a preventative and promotional sickness strategy for PD among UK women in their 50s and 60s. It gives some background on PD and explains why the topic was chosen. Statistics supporting the facts about PD in the UK’s targeted population have been provided by epidemiology. Subsequently, it evaluated the PD case, established targets, and suggested interventions to meet the goals. It concludes by assessing the suggested interventions’ efficacy and highlighting their advantages and disadvantages. My assessment establishes a solid basis for comprehending the complexity of Parkinson’s disease by offering a comprehensive background examination of health issues, types, and causes related to PD. The frequency, trends, and impacts of PD in the given population are clarified by epidemiological insights, underscoring the necessity of focused interventions. An essential component of care planning that helps with the early diagnosis and treatment of PD is nursing evaluation. Adopting health promotion models—the Health Belief Model in particular—provides a framework for comprehending people’s perceptions, beliefs, and obstacles associated with PD, directing the creation of customized therapies. Clear aims for improving outcomes and elevating the quality of life for people with PD can be provided by setting goals, such as creating a CBT hotline and encouraging positive lifestyle modifications. The goal of multimodal therapies, such as lifestyle changes and remote trials, is to treat both the motor and non-motor symptoms of PD, improving the mitigation and management of the disease. Evaluation is still necessary to determine whether an intervention is beneficial, and suggestions for improvement—like interdisciplinary cooperation and evidence-based methods—provide insightful information that can be used to improve interventions in the future.
References
Geng, T. et al. (2023). Social isolation and the risk of Parkinson’s disease: The UK biobank study [Preprint]. doi:10.21203/rs.3.rs-3310236/v1.
Janssen Daalen, J.M. et al. (2022). ‘Lifestyle interventions for the prevention of Parkinson disease’, Neurology, 99(7_Supplement_1), pp. 42–51. doi:10.1212/wnl.0000000000200787.
Parkinson’s UK (2020) Reporting on Parkinson’s: Information for journalists, Parkinson’s UK. Available at: https://www.parkinsons.org.uk/about-us/reporting-parkinsons-information-journalists#:~:text=Men%20aged%2050%20to%2089,50%20to%2089%2C%20have%20Parkinson’s. (Accessed: 28 March 2024).
NHS (2022) Diagnosis -Parkinson’s disease, NHS choices. Available at: https://www.nhs.uk/conditions/parkinsons-disease/diagnosis/#:~:text=Your%20doctor%20will%20base%20a,to%20help%20with%20the%20diagnosis. (Accessed: 28 March 2024).
Preparing for end of life: An emotional guide (2011). London: Parkinson’s UK.
Sturkenboom, I.H., Nijhuis-van der Sanden, M.W. and Graff, M.J. (2016). ‘A process evaluation of a home-based occupational therapy intervention for Parkinson’s patients and their caregivers performed alongside a randomized controlled trial’, Clinical Rehabilitation, 30(12), pp. 1186–1199. doi:10.1177/0269215515622038.
Tam, W., Alajlani, M. and Abd-alrazaq, A. (2023). ‘An exploration of wearable device features used in UK hospital parkinson disease care: A scoping review’, Journal of Medical Internet Research, 25. doi:10.2196/42950.
Todd, A.M. et al. (2016). ‘Good-quality social care for people with Parkinson’s disease: A qualitative study’, BMJ Open, 6(2). doi:10.1136/bmjopen-2014-006813.
Vallée, A. (2023). ‘Association between social isolation and loneliness with estimated atherosclerotic cardiovascular disease risk in a UK Biobank population-based study’, International Journal of Environmental Research and Public Health, 20(4), p. 2869. doi:10.3390/ijerph20042869.
‘Parkinson disease’ (2023) Palliative and Hospice Care Nursing Guidelines [Preprint]. doi:10.1891/9780826144485.0014d.
Donovan, H. & Warriner, J. (2017). Nurses’ role in public health and integration of health and social care. Primary Health Care, 27 (8), 20–24. Available from: https://www.researchgate.net/publication/320079417_Nurses’_role_in_public_health_and_integration_of_health_and_social_care [Accessed 27 November 2022]
Graham, H. and White, P.C.L. (2016). Social determinants and lifestyles: integrating environmental and public health perspectives. Public Health, 141 (2016), 270–278. Available from: https://www.sciencedirect.com/science/article/pii/S0033350616302505 [Accessed 26 November 2022]
Hussein, Z. A. and Saadoon, N.Y. 2021. Assessment of Nurse’s Challenges Regarding Health Care System in Hilla City. Annals of R.S.C.B., 25 (6), pp. 530-539.
Kayser, L., Karnoe, A., Duminski, E., Somekh, D. & Vera-Muñoz, C. 2019. A new understanding of health-related empowerment in the context of active and healthy ageing. BMC Health Serv Res, 19 (242), pp. 1-13. Available from: https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-019-4082-5 [Accessed 26 November 2022]
Michie, S., Atkins, L. & West, R. (2014). The behaviour change wheel: A guide to designing interventions. Sutton: Silverback Publishing.
Paton, M., Naidu, T., Wyatt, T.R., Oni, O., Lorello, G.R., Najeeb, U., Feilchenfeld, Z., Waterman, S.J., Whitehead, C.R., & Kuper, A. (2020). Dismantling the master’s house: New ways of knowing for equity and social justice in health professions education. Advances in Health Sciences Education, 1 (20), 1–16.
Ross, A., Bevan, M., Brooks, A.T., Gibbons, S. & Wallen, G.R. (2017). Nurses and health-promoting behaviours: Knowledge may not translate into self-care. AORN J.,105 (3), pp. 267–275. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5536335/ [Accessed 26 November 2022].
Scott, P. A, Harvey, C., Felzmann, H., Suhonen, R., Habermann, M., Halvorsen, K., Christiansen, K., Toffoli, L. and Papastavrou, E. 2019. Resource allocation and rationing in nursing care: A discussion paper. Nurs Ethics, 26 (5), pp. 1528-1539. Doi: 10.1177/0969733018759831.
Acharya, S., Salgado-Somoza, A., Stefanizzi, F. M., Lumley, A. I., Zhang, L., Glaab, E., … & Devaux, Y. (2020). Non-coding RNAs in the brain-heart axis: The case of Parkinson’s disease. International journal of molecular sciences, 21(18), 6513.
Ansari, I., El-Kady, M. M., Arora, C., Sundararajan, M., Maiti, D., & Khan, A. (2021). A review on the fatal impact of pesticide toxicity on environment and human health. Global Climate Change, 361-391.
Beckers, M., Bloem, B. R., & Verbeek, M. M. (2022). Mechanisms of peripheral levodopa resistance in Parkinson’s disease. npj Parkinson’s Disease, 8(1), 56.
Church, F. C. (2021). Treatment options for motor and non-motor symptoms of Parkinson’s disease. Biomolecules, 11(4), 612.
Franco, G. A., Interdonato, L., Cordaro, M., Cuzzocrea, S., & Di Paola, R. (2023). Bioactive Compounds of the Mediterranean Diet as Nutritional Support to Fight Neurodegenerative
Disease. International Journal of Molecular Sciences, 24(8), 7318.
Horn, A., Al-Fatly, B., Neumann, W. J., & Neudorfer, C. (2022). Connectomic DBS: An introduction. In Connectomic Deep Brain Stimulation (pp. 3-23). Academic Press.
Lee, C. Y., Menozzi, E., Chau, K. Y., & Schapira, A. H. (2021). Glucocerebrosidase 1 and leucine‐rich repeat kinase 2 in Parkinson’s disease and interplay between the two genes. Journal of Neurochemistry, 159(5), 826-839.
Lorking, N., Murray, A. D., & O’Brien, J. T. (2021). The use of positron emission tomography/magnetic resonance imaging in dementia: A literature review. International Journal of Geriatric Psychiatry, 36(10), 1501–1513.
Monge-Fuentes, V., Biolchi Mayer, A., Lima, M. R., Geraldes, L. R., Zanotto, L. N., Moreira, K. G., … & Mortari, M. R. (2021). Dopamine-loaded nanoparticle systems circumvent the blood-brain barrier, restoring motor function in mouse models for Parkinson’s
Disease. Scientific reports, 11(1), 15185.
Nebrisi, E. E. (2021). Neuroprotective activities of curcumin in Parkinson’s disease: a review of the literature. International journal of molecular sciences, 22(20), 11248.
Nestor, M. S., Arnold, D., & Fischer, D. (2020). The mechanisms of action and use of botulinum neurotoxin type A in aesthetics: Key Clinical Postulates II. Journal of cosmetic dermatology, 19(11), 2785-2804.
Pathania, R., Chawla, P., Khan, H., Kaushik, R., & Khan, M. A. (2020). An assessment of potential nutritive and medicinal properties of Mucuna pruriens: a natural food legume. 3Biotech, 10(6), 261.
Prenger, M., Madray, R., Van Hedger, K., Anello, M., & MacDonald, P. A. (2020). Social symptoms of Parkinson’s disease. Parkinson’s Disease, 2020.